
It’s hard for your Editor to believe, but this is actually the 15th year since Steve Hards was most kind and invited me to contribute a few articles to what was then simply Telecare Aware.
A lot has happened since then, professionally and personally. I’m grateful for the opportunity that TTA has given me to Cover the Healthcare Waterfront, relying on multiple sources from super-local to Mainstream News to the Usual Sources.
Most of all, this forum (and it is one!) stays true to the course that now Editor Emeritus Steve set some years ago:
Telecare Aware’s editors concentrate on what we perceive to be significant events and technological and other developments in telecare and telehealth. We make no apology for being independent and opinionated or for trying to be interesting rather than comprehensive.
In that, though I’ve occasionally gone far afield (and down some rabbit holes) into exclusively US issues such as how healthcare gets paid, its politics, and the financial landscape (from bubble to devastation to recovery), I believe they hold true in the UK and in other countries.
So one wish I have from Santa for 2025 is for More Comments. I’m very interested in knowing what you think about topics that are covered and your take on them. Using hits as a guide, it is hard to predict. Sometimes it is breaking news, a major data breach, or Walgreens’ continuing soap opera. Perhaps you want more audio commentary or article audio files, which I’ve experimented with via Soundcloud. So…What do you think?
A second wish: for other writers to join me here as lead/topic providers or better, contributors, for news outside the US. Specifically, I believe Readers want to know what is going on in the UK and Europe, but ‘standard sources’ are either not focused on health tech, paywalled, or overly specific ‘inside baseball’. Steve and I have long recommended Roy Lilley’s newsletter and UK Telehealthcare.
So…if you know of reporting on UK or EU issues, please direct me there. Better yet, contribute an article! Or two! We are small and cannot pay, but if the facts are there and the writing is sound, you’ll be published and can republish elsewhere. (This is exclusive of Perspectives, which are non-promotional thought pieces contributed by companies’ marketing areas. And we thank them!)
A third wish: speaking of marketing, I am a marketing and communications consultant by trade. Yet I am very shy about putting my shingle out there and asking Readers for leads to companies that might need marketing help, short-term or long term. My LinkedIn profile has most of my CV and key information on what I’ve done and where I’ve worked, but for a full overview about my capabilities across branding, program, planning, and products, email me here.
 Now for the Quirky Predictions–I’ll keep it short and open to debate:
Now for the Quirky Predictions–I’ll keep it short and open to debate:
2025 will continue international rebuilding of companies in healthcare and health tech. But the tear-downs will continue to clear the table. Overall, there’s optimism in the air with a new administration. It doesn’t feel like a rerun of 2023 where everyone thought it was going to be Romping Unicorns post-pandemic and the Big Guns were snapping up Big Buys like Signify Health and Oak Street Health for Big Bucks. We know now how that worked out for Walgreens, CVS, Walmart, and even Amazon (which I predict will be rethinking–and retrenching). We are starting from a low level and hopefully leveling up from there.
That doesn’t mean that there won’t be more Shotgun Mergers by VCs that avoid the new merger guidelines and a few Chapter 7s and 11s (UK=administration) along the way. There will be more layoffs. Funding rounds for both healthcare and digital health will be moderate. Down rounds that reduce valuation will still be with us. Investors will push for more control–witness what is happening at Walgreens and CVS, and what happened at Centene. There will be more big changes at Walgreens, CVS, Elevance, Centene, Cigna, and many others considered mainstays of healthcare–and don’t rule out Amazon and Walmart. But by the end of year, barring a Bird Flu Pandemic, space aliens landing from the Plague of Drones in US and international skies, or an Unraveling of Sanity, overall we will be doing a lot better.
Robert F. Kennedy Jr. will be turning up the heat on Health. He will be confirmed as head of Health and Human Services and will, within a year, refocus it along its name. Health rather than Sick Care. A lot of substances ranging from vaccines to PFAS to various dyes and additives in food will be questioned at FDA, restricted, and brought to the national consciousness. As a personality, he is extremely intelligent and dynamic–knows how to absorb the most complex information and move on it. He knows that Make America Healthy Again is his Main Chance and also to be true to his legendary father’s legacy. It will make a lot of drug and chemical companies rather…nervous. (I am less sanguine about Dr. Mehmet Oz as head of CMS and his ability to clean up that puzzle palace, but hopeful.)
Speaking of heat, I wouldn’t want to be a C-level at any of the major health plans that are in multiple lines of integrated business. The assassination of Brian Thompson and earlier the massive Change Healthcare hack ripped the cast and bandages off the entire system. The sheer hostility to payers was startling enough for UHG CEO Andrew Witty to write a massively defensive op-ed in the NY Times–and the hostility has hardly dimmed with the jailing of Luigi Mangione who has turned into a folk hero to some. (Yeesh! I cannot think of anything less moral.) The incoming administration and Congress are restive and major changes will be coming from there. Already there is a bipartisan Congressional bill (the PBM Bill) requiring the divestiture of pharmacy benefit management (PBM) companies from insurers within three years. While it will not be passed by the 118th Congress, it will be reintroduced by the 119th after 3 January if you look at who is backing it. This is the kind of movement to simplify how healthcare is delivered and paid for that crosses ideologies and finds a wide spectrum of support from Bernie Sanders to RFK, Jr. and presumably the re-elected President.
Once the PBM string is pulled, what then comes into focus is insurer ownership and control of providers. UHG/Optum owns or is affiliated (meaning ACO or partial ownership) with 10% of US practices. DOJ is already after UHG for the Change Healthcare acquisition on security grounds. The more aggressive posture around anti-trust will not change in this administration and only slightly moderate with a new FTC chair. (Lina Khan’s term has expired though she may try to hang on, but her bête noire Amazon is still in trouble with their One Medical Bad Bet.) The few payer organizations that only offer health plans, like Molina, Oscar, and Clover, will start to look very smart indeed. Perhaps smaller and less controlling is actually…better. And more profitable.
Running in parallel: the lack of trust in Big Pharma and the cost of drugs from them. They’re next.
We will need to get much more realistic about AI, what it is capable of, and its social effects. It is spreading into everything like kudzu (try entering into most browsers) but what we will be finding out is that a lot of what is ‘AI’ sold to companies as labor-saving is half-baked. It doesn’t work well. Some of it falls into the ‘uncanny valley’ of unease as too humanoid. If a company or service relies on it for decision making, it may not make those decisions better than humans. Reportedly UnitedHealthcare uses AI for a claims decision model, something that is cited as flawed. Bad decisions incite human anger, and lack of human contact is like being in a perpetual voice jail.
There is also growing evidence that in writing and researching, over-dependence on AI prompts and drafts destroys the ability to remember and creatively connect both on the fly and under consideration, in the ability to move an argument logically to a conclusion utilizing persuasive writing and speech skills. This especially affects the young. I’m hearing reports on this from the hiring front, where young grads cannot write without AI assistance and are stunted in their verbal skills. AI in writing gets to be a crutch (I use a tool for grammar–and about 10% of the time it’s off.). And have we forgotten that AI is dependent on content….GIGO from the early computing days still applies. We don’t want to be the Eloi, do we? (Look up your H.G. Wells)
And one last prediction. The mass market weight loss fad hyping GLP-1 drugs (Wegovy, Ozempic, Mounjaro, Zepbound) will implode. These drugs are now readily available, less expensive (but certainly not cheap), and cheerily advertised on social media, radio, and TV by drug manufacturers and telehealth prescribers. These are promoted for weight loss alone, not for weight loss to better manage Type II diabetes or true obesity. What will pop the bubble? Side effects of slow digestion like stomach paralysis. Diarrhea, nausea, intestinal distress, even pancreatitis and suicidal ideation. Little known is that 80-90% of clinical trial participants experienced at least one adverse event. If you survive these, a weight gain rebound often happens once off the injections.
The telehealth prescribers like Ro and Hims make it so easy–and do they go through blood and other testing, and histories, to ensure that the patient is a suitable candidate? Metabolic modifications ain’t beanbag.
A side business popping up: nutritional supplements and ‘special drinks’ to prevent malnutrition (because of the low food intake) and muscle loss. (Another sign that GLP-1 is hitting a peak.)
Perhaps waiting in the wings are the class action lawyers, ready to jump on any massive side effects or, God forbid, deaths.
No ‘craze’–and this is one–is unalloyed bliss. If you have a diversified telehealth company like Teladoc and you get into this business, it may not make a difference (?)–but sole providers like Calibrate (among many) will feel the pain. And destruction. (Does anyone remember the much-touted Alli/Orlistat that reduced the fat absorbed by the digestive tract and those side effects?)
May you and your loved ones have a Merry Christmas, Happy Hanukkah, and a Happy New Year…however you and yours celebrate! We will be on a two-week break and return, along with many of you, on 6 January.

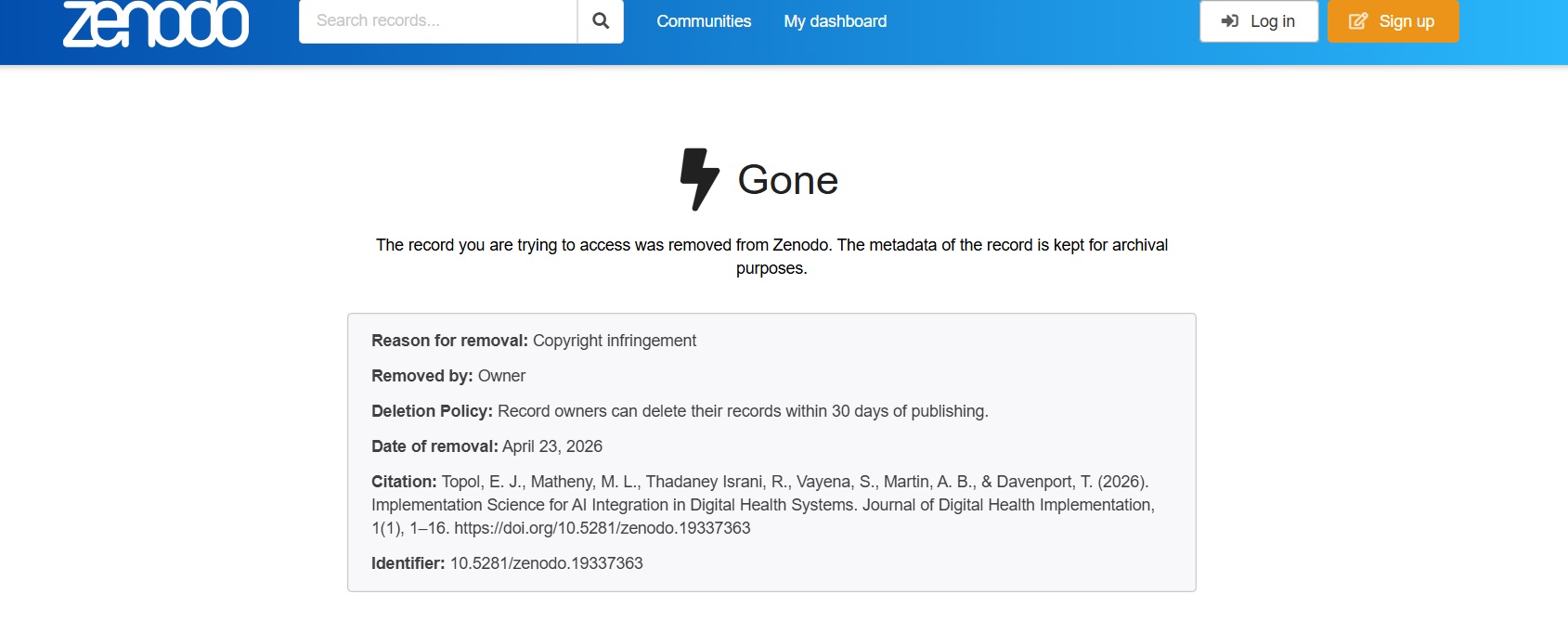
 From his post along with a screenshot of the ‘paper’ and a link:
From his post along with a screenshot of the ‘paper’ and a link:  Gemini came up with this about Ellinger: “Ellinger Publishing Media: An independent academic publisher specializing in open-access journals, specifically focusing on artificial intelligence, medicine, social sciences, and interdisciplinary research.” Again, links in the AI summary to e-pubmed.co.uk do not work. My conclusion is that this is a total spoof/hack using a URL similar to the former UK E-PubMed and this Ellinger Publishing is a fraud. I don’t know how you picked it up but it’s no longer reachable.
Gemini came up with this about Ellinger: “Ellinger Publishing Media: An independent academic publisher specializing in open-access journals, specifically focusing on artificial intelligence, medicine, social sciences, and interdisciplinary research.” Again, links in the AI summary to e-pubmed.co.uk do not work. My conclusion is that this is a total spoof/hack using a URL similar to the former UK E-PubMed and this Ellinger Publishing is a fraud. I don’t know how you picked it up but it’s no longer reachable.





















Most Recent Comments